One of the few perks of being a psychologist in a medical school (apart from occasionally running to a colleague to check a personal health matter) was talking to researchers about the real state of knowledge in any particular field.
The Middlesex Hospital Medical School, which started in 1746 and was subsumed into UCL in 1987, had a great talent for developing new services. In a very minor way I added to that trend by setting up, with two other colleagues, a national referral centre for post-traumatic stress disorder, which is still in operation as an NHS clinic.
However, of much greater importance was the clap clinic. At a time when the usual appellation was Venereal Disease, two clinicians got together and decided, over a glass of champagne, to move it from the dark basement to the full daylight. In 1964 Duncan Catterall established the first Chair of Genito-urinary Medicine at the Middlesex Hospital Medical School, and so when the first symptoms of a strange sexually transmitted disease showed up in the very early 80s, James Pringle House started seeing the first cases and was at the forefront of European research. I went to seminars, talked to colleagues, and sometimes met the guest speakers for a canteen lunch. The greater the expert, the quicker they were to admit that no-one knew what the hell was going on.
To my dismay, the public management of the disease quickly veered away from traditional public health concerns, and became a political battlefield. At the WHO headquarters in Geneva senior colleagues muttered that they had been criticised for saying the virus came from Africa: a colonialist perspective, they were told. Even years later, those who worked in the field in London talked sadly, and privately, of the difficulties they encountered with giving straightforward health warnings. I wanted to design a simple poster to illustrate the relative risks, but it got no further than a large page in my filing cabinet. Such, dear readers, were the difficulties of quickly disseminating an opinion before blogging became available.
It was clear to researchers that blood was the key vector of transmission (contaminated blood transfusions had a 90% chance of resulting in the recipient getting HIV), so that shared needle drug injecting and to a lesser extent anal intercourse without condoms were high risk activities, but public broadcasts talked vaguely about icebergs, and suggested everyone was at risk. I did some research on public perceptions of risk at that time, and AIDS figured high in the public mind. The common folk knew that it was a “gay plague” but the expert emphasis seemed to be on getting heterosexuals to use condoms. The great and the good were interviewed and asked to say the word “condom” on camera which they valiantly did. The correct way of putting on a condom was demonstrated on television, using a cucumber. This led to some worried calls about whether one could catch AIDS from a cucumber.
However, it was generally agreed that the UK government had done “rather well” and had got on top of the crisis. Now, with Ebola in the news, I thought it worthwhile looking at the current situation for the HIV virus in the UK, 30 years on from the first outbreak. This might give us a possible scenario for imagining what Ebola might look like in terms of prevalence.
In fact, the UK response to HIV seems to have been at the European average. Statistics vary in different parts of the world, but I imagine that European statistics have a modicum of accuracy. Finland, Germany, Malta, Norway (and Cuba, see below) did very well (0.1 %); Denmark, Greece, Netherlands and Sweden and Israel pretty well (0.2%) and Belgium, Iceland, Ireland, Luxemburg and the United Kingdom were average (0.3%). Austria, France, Italy, Spain, Switzerland were a bit worse (0.4 %) and Portugal very much worse (0.7%). Of course, these are not sub-Saharan African levels (as high as 25% in Swaziland and Botswana) but given that the governments knew what was coming, and had resources available, they are not stellar achievements.
Greg Cochran mentioned the case of Cuba, which had forewarning of the virus in the US and two years to prepare for their first case.
http://westhunt.wordpress.com/2014/09/28/forty-days/
They quarantined patients for 8 weeks of health education, tracked contacts in a very determined way, and used their relative isolation to put public health before private liberty, an approach which comes naturally to the regime. Their resultant prevalence of roughly 0.1% is one-sixth the rate of the United States, one-twentieth of nearby Haiti.
http://news.bbc.co.uk/1/hi/in_depth/sci_tech/2003/denver_2003/2770631.stm
HIV probably moved from monkeys to humans before the 1950s, although the first cases were recognised in 1981 in the US. About 100,000 people in the UK are infected, mostly homosexuals, and heterosexuals from sub-Saharan Africa. More than 20 per cent of them do not know it, and are several times more likely to transmit the virus to their partners than those who have a diagnosis. Half of the newly diagnosed cases in the UK seek medical help when they are in the late stages of disease. In 2012, there were 6,360 new diagnoses of HIV, which is 17 a day in case you find that more dramatic. In England the local authorities with the highest prevalence of diagnosed infections are London, Brighton and Hove, Salford, Manchester, Blackpool and Luton, and in Scotland, Edinburgh. Treatment with antiretroviral drugs reduces the risk of transmission by more than 90 per cent. The cost of these drugs is said to be £20,000 a year and given the current almost normal life spans of HIV patients, 20 years of medication seems a prudent minimum for budgeting purposes. The money spent per capita on NHS services in England was £1,979 in 2011, so each patient with HIV consumed at least 10 times the resources of an average patient every single year.
http://www.avert.org/uk-hiv-aids-statistics.htm
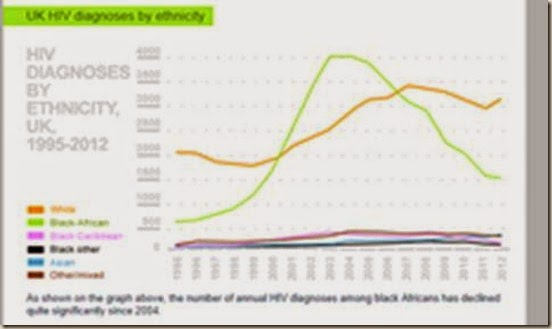
A possible explanation for the apparently lacklustre performance of the UK may be that many of the cases are imported: that is, brought in by Black Africans infected in Africa. Looking at the demographics of the UK in 2011 that shows that 55,730,000 persons are classified as White and 1,905,000 are classified as Black or Black British. Looking at the HIV figures (this is broad brush, because I have omitted the “mixed” groups) the HIV rates per 100,000 are as follows:
Whites: 93 per 100,000
Blacks: 2015 per 100,000
So, the rate seems to be 21 times higher among Africans. The fact that so many Africans have come to the UK cannot be blamed on the quality of UK public health warnings aimed at changing the behaviour of the local population. The White rate is exactly comparable with the best European nations at 0.1%
Nonetheless, considering that about 36 million people in the world are infected by HIV and that 30 million have died, the management of HIV is hardly a global success story. Does this give us any help in looking ahead to the prevalence of the Ebola virus in 30 years’ time? Prediction will depend on whether treatments or vaccinations become available, but my impression, no more than that, is that the spread of the virus should be much slower, very much slower. HIV can be passed on whilst the carrier still looks good for sex, and sex is fun, so HIV gets an easy ride. Ebola can only be passed on (if the experts are right) when the carrier is looking pretty ill and unattractive, and dealing with ill people is a duty, and not much fun. Furthermore, Ebola is so virulent at the moment that immediate death rates are high. With simple precautions it should be contained. Even when “protocols” fail, the reproduction rate of the virus in human carriers should be low. Despite all the worrying news, it should be a simple matter to avoid the spread of the disease.
On a more speculative note, perhaps we shall be saved by stigma. By fearing all people who look as if they are ill with Ebola, stigmatising them and avoiding all contact with them, definitely not putting ourselves at risk by helping them, particularly not touching them when they are dying or dead, the virus will die out. So, in one corner we have the virus, in the other corner the uncertain public, caught in an awkward tussle between altruism and abject fear. Ebola has its best chance of spreading in societies which don’t believe it exists (like in parts of Africa), and to a lesser extent in those which don’t believe that, given the virus does exist, the absolute priority is to change our behaviour quickly (parts of the wealthy West). Informed opinion ought to be right, but with every failure of both treatment and containment in Western hospitals public belief is eroded.
Although it goes against altruistic instincts, futile attempts at interventionist treatments may be making matters worse.

I agree entirely. I often think that much of our ethical attitudes have arisen from a sort of culture of nobility where money is no object and the unknown is completely within our power. Now that our economies flounder, our dreams of space colonization wither, and our antibiotics fail, we're only beginning to realize that attempts at creating a perfect world may be unworkable. But without perfection to shoot for, many people I talk to don't seem to know where to set their sights.
ReplyDeleteYes, it might be that we need "perfection to shoot for". In a more prosaic way, modern medicine often battles to save a life without considering the consequences. Low birth weight babies are a case in point: their outcomes can often be poor, but no-one is all that bothered about it. Much of it depends on being seen to be helpful at the time, and not thinking further.
ReplyDelete