I have delved into this issue before, saying that psychiatrists (the missionaries) were torn between trying to normalise mental illness, and (the actuaries) admitting that some psychiatric illnesses have deleterious effects on behaviour, particularly an increase in violence.
http://drjamesthompson.blogspot.co.uk/2013/03/schizophrenia-and-violence-delusional.html
http://drjamesthompson.blogspot.co.uk/2013/09/bad-blood.html
Now there are startling new results from a large, representative sample of Norwegians, showing that the rate of violence is about 7 times higher in schizophrenics as compared to controls, and 3 times higher for those with bi-polar disorder.
Genetic and environmental determinants of violence risk in psychotic disorders: a multivariate quantitative genetic study of 1.8 million Swedish twins and siblings
OPEN
Molecular Psychiatry advance online publication 15 December 2015; doi: 10.1038/mp.2015.184
A Sariaslan, H Larsson and S Fazel seena.fazel@psych.ox.ac.uk
Advance online publication 15 December 2015
http://www.nature.com/mp/journal/vaop/ncurrent/full/mp2015184a.html
Amir Sariaslan, formerly at the Karolinska, and now with colleages at Oxford, is becoming known for delving into the large goldmine of Swedish epidemeolgy and coming up with sparkling nuggets.
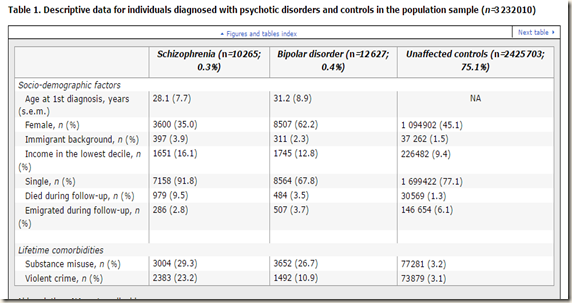
These are startling figures, based on excellent and very large samples, showing very high levels of substance abuse for schizophrenia and bipolar disorder, and high rates of violence for both, but particularly schizophrenia. Women seem to get bipolar disorder, men schizophrenia. Immigrants are slightly over-represented in bipolar and over twice as likely to get schizophrenia, a commonly found pattern. Schizophrenia particularly damages employment prospects and marriage prospects.
We observed, for instance, that nearly one in four (23%) schizophrenia patients had ever been convicted of a violent crime, whereas the equivalent prevalence was 11% in patients diagnosed with bipolar disorder and 3% in controls.
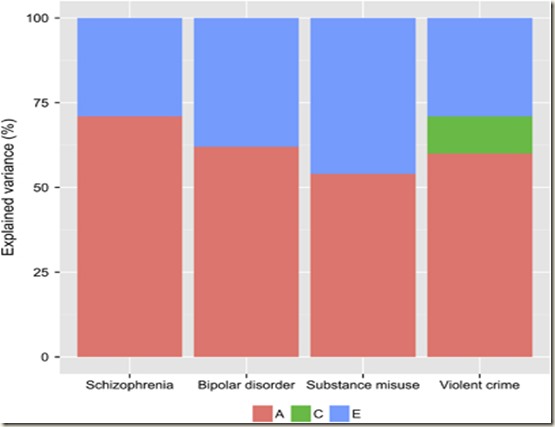
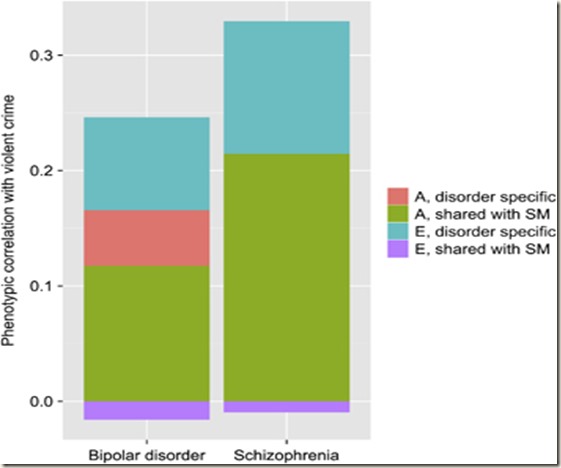
Schizophrenia was a stronger predictor of violent crime (r=0.32) than bipolar disorder (r=0.23). Consistent with previous quantitative and molecular genetic studies demonstrating important pleiotropic effects between the examined phenotypes,13, 14, 15 we found that 67% of the correlation between schizophrenia and violent crime, and 51% of the correlation between bipolar disorder and violent crime was attributed to additive genetic influences that were shared between the psychotic disorders, substance misuse, and violent crime. This suggests that the increased risk for violence in these patient groups could largely be attributed to the same genetic factors that simultaneously increased their liabilities to substance misuse and to be diagnosed with the psychotic disorders in the first place. However, we additionally observed a novel finding in that the additive genetic influences that were unrelated to substance misuse explained approximately a fifth (21%) of the correlation with violent criminality in bipolar disorder but none of the same correlation in schizophrenia. In other words, we found support for the existence of disorder-specific genetic effects linking bipolar disorder (but not schizophrenia) to increased violence risk. This implies that aetiological models involving psychotic disorders should not only focus on genetic and environmental factors that are shared between the disorders but also on those factors that are unique to each disorder.
Once again, very little shows up for C, the shared variance of family life we used to think had such an influence.
Here are the two disorders on their own, showing high heritability together with substance abuse, something disorder specific for bi-polar, and unique disorder-specific variance for both.
The authors are circumspect about the implication of their findings. They observe: Clinically, these findings illustrate the importance of risk assessments that consider substance misuse comorbidity, integrated treatments for multiple adverse risks and strong collaborations between criminal justice, substance misuse and mental health services.
If nearly one in four schizophrenics are convicted of violent crime then both the problem and the solution are now much clearer. I had formerly believed what I had been told, which is that violence was so rare in psychosis that it could not be prevented, other than by restricting the freedom of a very large number of schizophrenic patients. These findings suggest that for every schizophrenic patient closely monitored for substance abuse and aggressive behaviour 3 patients will be mildly restricted, a very tolerable ratio. This, in my view, totally changes the Number Needed to Treat calculation in favour of close monitoring. We routinely suggest treatments where the numbers needed to treat are 10 or higher. So long as the coordinated treatment regime were properly managed, few interventions would be show such extraordinary returns on treatment.
I do not want to stigmatise psychiatrists who deal with schizophrenic patients, but they now have a different calculation to make, and new findings to discuss with secure ward hospital administrators and, most of all, legislators. There is a case for preventative medicine in psychosis. This is nothing to do with stigmatisation and a lot to do with evidence-led interventions.

I spent some time as a psychiatrist and was crystal clear that psychosis (whether or not it gets the vague label of schizophrenia) makes some people violent who might otherwise not be - of this there is no question.
ReplyDeleteI recall a quiet, small, sweet mother of young children who - when manic - launched unprovoked violent attacks on the nursing staff. Melancholic depressed mothers may smother their beloved children then kill themselves (to save the children from what they perceive to be an utterly miserable world). Catatonic patients have been known to kill staff in frenzied attacks out of the blue and without any motivation.
There should not be any controversy about this! The factors which affect the possibility of violence should be well known - they include, male sex, youth, class, race, intelligence, drugs (especially androgenic steroids) - and psychotic illness (including some forms of brain damage, dementia and delirium).
Social class does not cause violent crime, at least not in Sweden. We've examined the effects of neighborhood deprivation, as well as family income/welfare recipiency, and the findings indicate that the observed associations on the population-level are entirely explained by familial selection factors:
Deletehttp://www.ncbi.nlm.nih.gov/pubmed/24062294
http://www.ncbi.nlm.nih.gov/pubmed/25147371
James was kind enough to blog about the latter study when it came out last year: http://drjamesthompson.blogspot.se/2014/08/depraved-on-account-of-being-deprived.html
@AS - In real life, confounders are not adjusted-for!
DeleteSchizochristian talking about lunacy of their patients.
DeleteWhat world is that???
(i) Is it a fair guess that any inaccuracy in diagnosis dilutes the effects - in other words, the effects would look even bigger if diagnosis were perfect?
ReplyDelete(ii) Even as it stands, the numbers seem to support the current methods of diagnoses - these would appear to be real conditions.
As I've remarked before I've twice had to deal with a student falling into schizophrenia: it is a chilling business. All my pity was useless: I suppose pity often is. It's a fragile affair, human life.
Dear dearieme,
Delete(i) Yes, measurement error dilutes associations down to null. In the current study, we conducted complementary sensitivity analyses to test whether broader definitions (e.g., at least 1 episode) of the psychotic disorders impacted on the reported findings but they did not (see Supplementary table 5).
(ii) Yes, I agree. See also Pettersson's work and their discussion about how nationwide patient registry data on psychiatric disorders often converge with data from symptom-based (sub-)clinical samples http://www.nature.com/mp/journal/vaop/ncurrent/abs/mp2015116a.html
>All my pity was useless: I suppose pity often is. It's a fragile affair, human life.
DeleteYou're looking at it too simplistically. Most of the time, happiness depends on feeling loved by the people who are close to you. But if your appendix hurts, happiness depends a lot more on getting to a surgeon in a timely manner.
Similarly, pity is a wonderful gift, but there are situations when a sedative is a more appropriate gift.
I think the substance abuse needs to be examined in the context of generally high alcoholism in Sweden. I'm not too familiar with the culture, but I think they have a lot of alcoholics and a lot of puritans.
ReplyDeleteSo one possible explanation for this is that the schizos regress to Sweden's national pastime more often.
nice info mr
ReplyDeleteAm one of the happiest Father on earth,My son onces suffered from the problem Schizophrenia which made him not to go to school,and that was killing his educational carrier.he can not control his emotions,always having nosies on his head affect how he thinks, feels and acts,he has taken different medication,but no cure,then i got the contact of a doctor who helped my son. he gave me the medication which my son used, he took the medication for two weeks,and that was the end of the problem.he can now control his emotions,no more severely distorted self-image and feeling worthless acts, his thinking is normal and no more voices on his head any more.any one that need his medication should contact the Doctor on benardleo13@gmail.com
ReplyDeleteSchizophrenia has no cure,but I got the medication which am using for my son now,and he his already living fine and a normal life, he is also going to school now,you too can get the medication from Dr Ben by contacting him on benardleo13@gmail.com
ReplyDeleteWe think your information is much handy to me. When you keep going the perfect job i’ll come back at your weblog.
ReplyDeleteSchizophrenia Treatment Services
Schizophrenia has been a problem to my husband for fifteen years, he I have used different medication on him without any solution, I got the cure to Schizophrenia from Dr Ben, his product is made from herbs, and that was what i used on my husband, and now he is living like every other human,am the happiest woman on earth.there is no more hearing or seeing things that is not there,
ReplyDeleteany body with the same issues should contact Dr Ben at benardleo13@gmail.com
This was how i got a cure for my son who was diagnosed with schizophrenia 9 years ago when he was 19. He told us that he got messages and he heard people telling him that he should hurt himself. He had a terrible temper with cursing and violence towards me and his dad. The doctor gave him different anti-psychotic drugs like Zyprexa, prolixin, risperidone, Ablify but all this even elevated the condition because he became worse over the years not until last two years that help came our way. I got Dr Joseph's contact from an old colleague of mine who relocated to Kansas city and he told me about this herbal medicine that can put an end to my son's condition. I contacted the doctor and i explained it all to him and he told me all will be well. I got the medicine and gave him as instructed and before i knew it he was normal again, no side effects at all. I am writing this today because i needed to be sure the cure was a permanent one which it is. I know what schizo is and how heart aching it can be but i tell you today that there is a cure for it. Contact the doctor on (josephakormah@gmail.com) for psychosis, schizophrenia, bipolar disorder, he can help you too
ReplyDeleteI decided to share this to help someone out there who is still held with schizophrenia.
ReplyDeleteMy son suffered from chronic schizophrenia for 18 years and we traveled round the world from one hospital to another neurologist and spent thousands of dollars and even got scammed in this process of seeking a cure and the problem still persisted. He acted weird and aggressive and this was so scary. All thanks to Dr Joseph who was able to use his medicine to cure him permanently. He is one of the Honest men out there. If you want to contact him on how to get his medicine or for info just reach him directly on josephalberteo@gmail.com Thanks admin.
Looking for natural medicine to schizophrenia without any side effect Dr. Williams is the best because it has no side effect, After my son being diagnosed of schizophrenia in 2010, I have used numerous medicine for him with no improvement. He spent most of the summer in the hospital. I remember him feeling abandoned and terrified of the many injection needles that seemed necessary to keep him calm. All Western Medicine used in the past did not have any noticeable difference,one day as i was going through the internet i came across so many people with different disease testifying about dr williams herbal remedies,i ordered for it on line,that's when he started using dr williams Herbal Medicine,and now is completely cured from schizophrenia , his medicine is a permanent cure to schizophrenia, for more info contact (drwilliams098675@gmail.com for advice and for his product
ReplyDelete