The geography of illness has never entirely convinced me, because people move about. So, finding an excess of some disorders in sunny coastal locations may have nothing to do with the local rocks, soils and water courses, and everything to do with pensioners retiring to sea-side resorts.
Humans are difficult to study, not only because they move about, but because they forget things; tell little and big lies; promise to take their tablets and to avoid salt, sugar and random sex but then do nothing else; won’t take part in studies, or take part and then drop out; change addresses and sometimes surnames; leave the country and then come back again; and all these foibles are exacerbated if they are mentally distressed and cannot keep track of things.
What is one to make of the finding that bad neighbourhoods have a larger than usual number of schizophrenic patients, or that studies of schizophrenic patients find that they often live in poor neighbourhoods? One interpretation is clear: that as their condition worsens they drop down the social hierarchy. The other interpretation is that bad living circumstances either create or worsen their condition. As usual, both interpretations have their adherents.
Into this dispute steps Amir Sariaslan and colleagues, marshalling enormous datasets with familiar aplomb to conclude that…… the diagnosis precedes the fall, and 65% of the effect is heritable. That is to say, that a range of heritable characteristics in the general population (including schizophrenia and also cognitive impairment) accounts for 65% of the effect of ending up in a poor neighbourhood.
http://www.nature.com/tp/journal/v6/n5/abs/tp201662a.html
A Sariaslan, S Fazel, B M D'Onofrio, N Långström, H Larsson, S E Bergen, R Kuja-Halkola and P Lichtenstein
Schizophrenia and subsequent neighbourhood deprivation: revisiting the social drift hypothesis using population, twin and molecular genetic data
Translational Psychiatry (2016) 6, e796; doi:10.1038/tp.2016.62
Published online 3 May 2016
Neighbourhood influences in the aetiology of schizophrenia have been emphasized in a number of systematic reviews, but causality remains uncertain. To test the social drift hypothesis, we used three complementary genetically informed Swedish cohorts. First, we used nationwide Swedish data on approximately 760 000 full- and half-sibling pairs born between 1951 and 1974 and quantitative genetic models to study genetic and environmental influences on the overlap between schizophrenia in young adulthood and subsequent residence in socioeconomically deprived neighbourhoods. Schizophrenia diagnoses were ascertained using the National Patient Registry. Second, we tested the overlap between childhood psychotic experiences and neighbourhood deprivation in early adulthood in the longitudinal Twin Study of Child and Adolescent Development (TCHAD; n=2960). Third, we investigated to what extent polygenic risk scores for schizophrenia predicted residence in deprived neighbourhoods during late adulthood using the TwinGene sample (n=6796). Sibling data suggested that living in deprived neighbourhoods was substantially heritable; 65% (95% confidence interval (95% CI): 60–71%) of the variance was attributed to genetic influences. Although the correlation between schizophrenia and neighbourhood deprivation was moderate in magnitude (r=0.22; 95% CI: 0.20–0.24), it was entirely explained by genetic influences. We replicated these findings in the TCHAD sample. Moreover, the association between polygenic risk for schizophrenia and neighbourhood deprivation was statistically significant (R2=0.15%, P=0.002). Our findings are primarily consistent with a genetic selection interpretation where genetic liability for schizophrenia also predicts subsequent residence in socioeconomically deprived neighbourhoods. Previous studies may have overemphasized the relative importance of environmental influences in the social drift of schizophrenia patients. Clinical and policy interventions will therefore benefit from the future identification of potentially causal pathways between different dimensions of cognitive functions and socioeconomic trajectories derived from studies adopting family-based research designs.
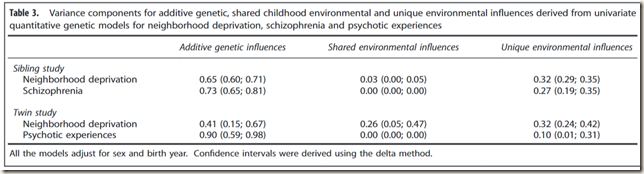
The study confirms in considerable detail what I had always regarded as highly likely, simply from observation of the the life course of schizophrenia, namely that as the condition progresses then sufferers are less able to make any contribution, and fall in their living circumstances. Second, yet another study shows that shared environmental influences are either zero or fairly small, which goes against the whole environmentalist creed, which I for one had always assumed was a reasonable explanation for the non-inherited chunk of the variance. The reality seems to be that things are for the most part inherited + random/unique. Here is table 3 ranked by additive genetic influence:
Psychotic experiences .90
Schizophrenia .73
Deprivation .41 - .65
Having psychotic experiences is very highly heritable; having the diagnosis of of schizophrenia also highly heritable; and ending up into a deprived neighbourhood also is heritable.
This paper ought to be seen as a definitive finding, although of course no finding is the final word. It will be interesting to see whether it is accepted within the social sciences as being the strongest contemporary explanation for why people end up in bad neighbourhoods.
(i) I wonder why evolution hasn't rid us of schizophrenia.
ReplyDelete(ii) Another example of Eysenck being right on the big picture, of nature triumphing over nurture.
(iii) The Best Journalist Currently Writing - the American blogger Steve Sailer - says (I paraphrase) that the worst curse of being poor is having to live among poor people.
(iv) How have you coped, doc, with a career of being immersed in such depressing stuff? It's bad enough that the truth is so sad, it must be worse that so many people who claim to be searching for the truth devote their careers to suppressing the truth as much as they can, thus obstructing attempts to deal intelligently and sympathetically with life's woes.
Perhaps, there's the rub for Psychology. We are humans studying other humans (and therefore, ourselves). Once you start looking at the material covered on this blog, you can understand why people in successful societies from the past were so cautious about human nature, and built societies (I am thinking of 19th and early 20th Century England for example) that were based on assumptions around needing to strictly guide human development and behaviour, for the common good. We know 'human kind cannot bear very much of reality' - but, ignoring reality could take us into the territory of Jim, who ran away from his nurse in the Belloc tale. Maybe, ignoring reality is far worse? Not everyone has the stomach for it tho' - or rather, not everyone has the combination of cognitive abilities and personality traits!
DeleteWotcha, doc. A Sailer commenter linked to this, which looks to be up your street.
ReplyDeletehttp://www.theatlantic.com/magazine/archive/2016/07/the-war-on-stupid-people/485618/
Rather than bother to correct the errors I welcome that, under cover of criticism, it shows the importance of intelligence. On balance, by contemporary standards of public discussion of intelligence, this will be informative.
Delete